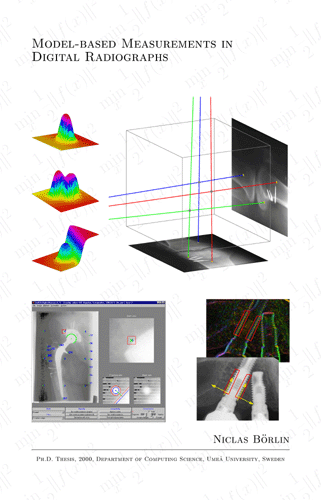
Model-based Measurements in Digital Radiographs
 Ph.D. Thesis, 2000, Department of Computing Science, Umeå University,
Sweden.
Ph.D. Thesis, 2000, Department of Computing Science, Umeå University,
Sweden.
Abstract
This thesis is about measurements in radiographs from two medical
applications; orthopaedics and prosthetic dentistry. However, some of
the methods and theory also applies to other types of images.
The thesis is divided into seven parts; papers I-V and appendices A-B.
Papers I-IV and appendices are related to Radiostereometric
Analysis (RSA), a stereographic measurement method used mainly in
orthopaedics. RSA is today the method of choice for studies of
micromotion and wear of orthopeadic implants in vivo. RSA is
based on markers implanted into the patient. Classically, the
measurements of marker coordinates in the X-ray films have been
performed manually using a high-precision measurement table. Paper
I describes a technique for performing the measurements in digital
radiographs, where a non-linear model of the image intensity near a
marker is least squares fitted to image data. Models of different
scenarios are presented, including a model of a nearby interfering
edge. The setup also facilitates selective exclusion of individual
pixels. In Paper II, the measurement method in Paper I
is shown to maintain or improve the clinical precision of the overall
RSA method compared to manual measurements as measured by double
examinations of knee and hip patients. These results are consolidated
in Paper III, which concentrates on RSA examination using the
uni-planar cage. The observer dependence is also studied. Paper
IV presents an effort to model the photogrammetric calculations
throughout the whole RSA method, including the reconstruction of the
projection geometries and motion calculation.
Paper V presents a method for alignment of intra-oral
radiographs for subtraction radiography, where the dental implant
under study is utilized as a reference object. A simple geometric
model of the projected thread outline is fitted to the image. A
coordinate system is defined based on the model fit and used to
provide a geometric correction between two exposures of the same
implant. The physical size of the implant is used to normalize the
coordinate system, making it possible to define regions of interest in
physical units relative to the implant. The method is shown to be
insensitive to a large variation of exposure conditions
in vitro. Together with a standard method for contrast
correction, the method is shown to be able to detect clinically
invisible simulated bone density changes near the implant.
Appendix A is included as an example of what RSA is used for
and how it is presented to the orthopaedic community.
Appendix B is included to indicate the programming effort behind
the measurement program in RSA that is another result of the work
behind this thesis.
Last modified: Tue Jul 25 13:38:58 MET DST 2000
 Ph.D. Thesis, 2000, Department of Computing Science, Umeå University,
Sweden.
Ph.D. Thesis, 2000, Department of Computing Science, Umeå University,
Sweden.